ARTICLES
Pre-Surgical Physical Therapy in Patients Undergoing Total Knee Replacement
Total Knee Arthroplasty (TKA) is the preferred treatment for patients with end-stage knee osteoarthritis (OA), inflammatory arthritis, or osteonecrosis when pain and functional disability persist despite conservative treatments. Preoperative pain levels, physical fitness, and impairments are strong predictors of knee function after TKA. Better preoperative knee function and fitness contribute to a smoother and faster postoperative recovery.
Patients are often referred to physical therapy before surgery to complete pre-surgical rehabilitation aimed at reducing limitations and improving range of motion (ROM) and strength, which can enhance outcomes after surgery.
A systematic review examining the effects of pre-surgical rehabilitation found the following benefits in the preoperative period across eight trials:
- Strength improvements in 75% of studies
- Enhanced performance in functional tasks such as the Timed Up and Go (TUG) and Sit-to-Stand (STS) tests in 66%
- Increased range of motion in 50%
- Reduced pain levels in 66%
- Improved health-related quality of life (HRQOL) in 33%
No significant changes were noted in stair climbing or walking tests preoperatively. Postoperatively, six trials reported favorable short-term effects on knee function:
- One trial showed significant strength gains
- Two trials showed improvements in TUG and ROM
- One trial noted HRQOL improvements
- Two trials demonstrated reduced pain levels
These benefits were observed up to three months after TKA, supporting improved recovery. While these short- and mid-term benefits are promising, evidence on long-term maintenance remains limited and of low to very low certainty.
Both clinicians and patients may consider prehabilitation as a valuable strategy to enhance short- and mid-term recovery following total knee replacement.
Reference:
Granicher, Pascale, et al. Prehabilitation Improves Knee Functioning Before and Within the First Year After Total Knee Arthroplasty: A Systematic Review with Meta-analysis. Journal of Orthopaedic and Sports Physical Therapy, Vol. 52, No. 11, 2022.
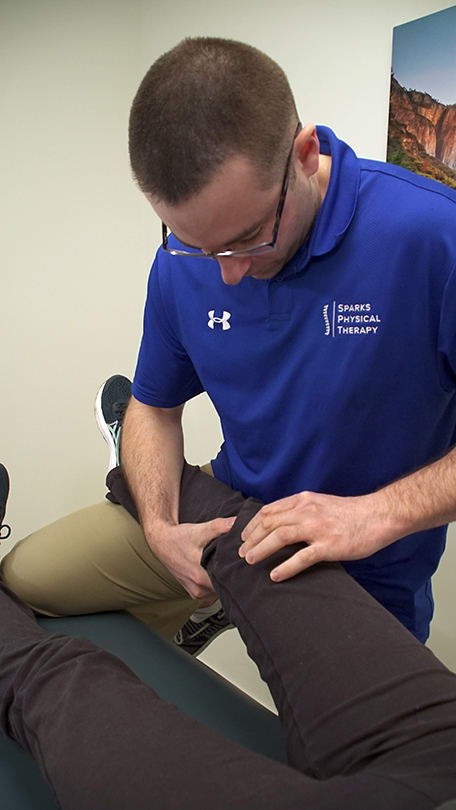
Physical therapist performing knee mobilizations.

Physical therapist providing manual therapy to improve knee flexion range of motion.

Physical therapist teaching a squat to improve knee mobility and strength.
Related Articles
Pelvic Floor PT/OT Interoception
Interoception is not a word that many people are familiar with, but it can be a key part in helping both adult and pediatric pelvic floor clients learn to address their pelvic floor symptoms and independently manage their pelvic floor needs during and after discharge from therapy.
Urinary Leakage and Incontinence
Urinary leakage and incontinence can occur for many different reasons. Some people leak urine in response to an increase in pressure in the abdomen either from a laugh, sneeze, or cough or from lifting, jumping, or running. Other people leak in response to a sudden, uncontrollable urge to urinate or a “bossy bladder.” As pelvic floor therapists, we treat and approach these kinds of incontinence differently.
Pelvic Floor PT/OT Diaphragm and Pelvic Floor Connection
The relationship between the pelvic floor and the diaphragm is often important when considering conditions like urinary incontinence, constipation, pelvic organ prolapse, and diastasis recti. When thinking about the abdomen like a canister, the pelvic floor is at the bottom of the canister and supports the abdominal contents and pelvic organs (rectum, uterus, and bladder) from the bottom.
