ARTICLES
Low Back Pain – Case Report (1) – (Radiculopathy, Extension Bias)
History: The patient presented with left-sided sciatica that began a couple of weeks ago. He reported a similar episode 2-3 years prior, which resolved with the use of a tennis ball and trigger point release. This time, the patient attempted trigger point release and stretching but felt these interventions actually worsened the pain. The pain was localized to the left lower gluteal region and intermittently radiated down to the left calf. At its worst, the pain rated 8/10; at its best, 2/10. The pain was described as sharp and shooting, most notably triggered by rising from a chair.
The patient has a history of advanced prostate cancer and recently completed radiation therapy. A recent PET scan was done, and he remains on hormone therapy. An active individual who enjoys skiing, the patient was hopeful to return to skiing with winter approaching. Despite the pain, he has maintained his workout routine without aggravating symptoms.
Functional Limitations:
- Getting up from sitting
- Bending forward in sitting position
- Pain with bowel movements
- Unable to perform recreational activities including skiing
Objective Finding:
- Lumbar active range of motion- Flexion 30deg, Extension 30sec, sidebending B 20deg. Pain with active lumbar flexion.
- Increased pain with repeated lumbar flexion testing and decreased pain with repeated lumbar extension.
- Myotomes- normal
- Dermatomes- normal
- Positive L slump and straight leg raise noting positive neural tension.
- Moderate tenderness and increased tone in L gluteus medius with referred pain to posterior upper thigh.
- Lower lumbar hypomobilty with CPA testing however no reproduction of pain.
Diagnosis: The patient was diagnosed with left lumbar radiculopathy with an extension bias. No sensory or motor deficits were noted. Treatment was initiated with extension-based exercises and neural mobilizations as part of the home program. The patient was also advised to use lumbar support while sitting.
Treatment:
- Manual Techniques started with trigger point release to increased tone in L gluteus medius and lumbar PA mobilizations. As tenderness and tone decreased focused on other mobilizations techniques including sidelying opening mobilizations, long axis distraction and passive L hip internal rotation and external rotation stretches.
- Exercises started with focus on lumbar extension based exercises, nerve glides and core stabilization. Addition of thoracic and lumbar flexion and rotation mobility exercises as pain decreased.
- As symptoms improved, patient was able to progress with weighted squats and deadlifts to prepare for ski season. Patient was also able to progress to higher level core strengthening exercises without increased pain.
Results: The patient was seen for a total of 8 visits. At the final appointment, he demonstrated a 25-degree improvement in lumbar flexion active range of motion and a negative straight leg raise. The slump test remained positive, and he continued to report very mild pain during bowel movements. However, the patient no longer experienced pain when rising from a seated position and was able to progress with deadlifts and cleans at home without exacerbation of symptoms. Unfortunately, the patient canceled his final visit, and follow-up through return to skiing was not completed.
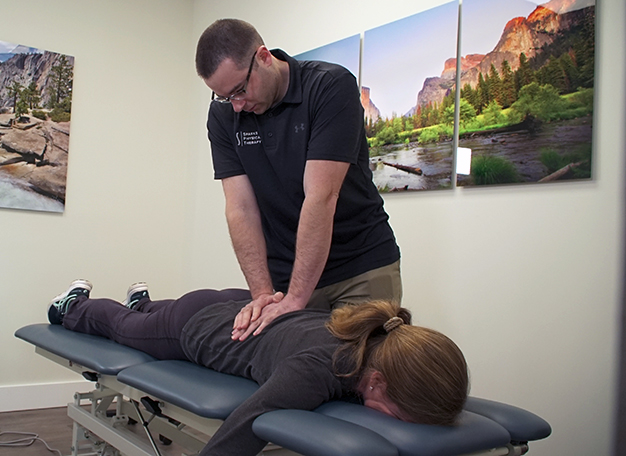
Physical therapist testing patients lumbar vertebral mobility.
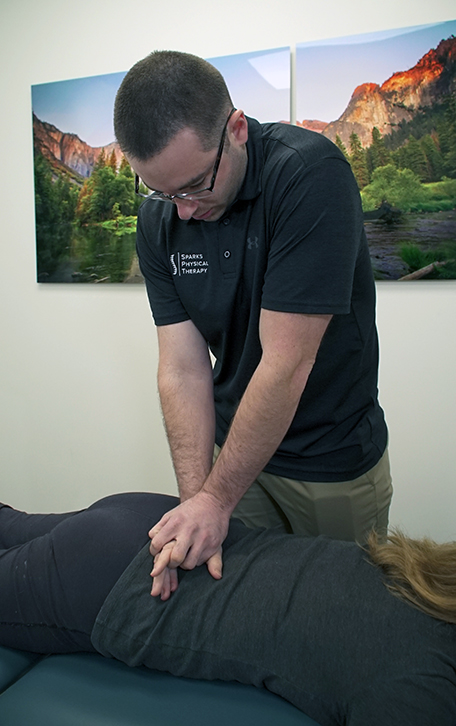
Lumbar PA mobilizations
Related Articles
Pelvic Floor PT/OT Interoception
Interoception is not a word that many people are familiar with, but it can be a key part in helping both adult and pediatric pelvic floor clients learn to address their pelvic floor symptoms and independently manage their pelvic floor needs during and after discharge from therapy.
Urinary Leakage and Incontinence
Urinary leakage and incontinence can occur for many different reasons. Some people leak urine in response to an increase in pressure in the abdomen either from a laugh, sneeze, or cough or from lifting, jumping, or running. Other people leak in response to a sudden, uncontrollable urge to urinate or a “bossy bladder.” As pelvic floor therapists, we treat and approach these kinds of incontinence differently.
Pelvic Floor PT/OT Diaphragm and Pelvic Floor Connection
The relationship between the pelvic floor and the diaphragm is often important when considering conditions like urinary incontinence, constipation, pelvic organ prolapse, and diastasis recti. When thinking about the abdomen like a canister, the pelvic floor is at the bottom of the canister and supports the abdominal contents and pelvic organs (rectum, uterus, and bladder) from the bottom.
